
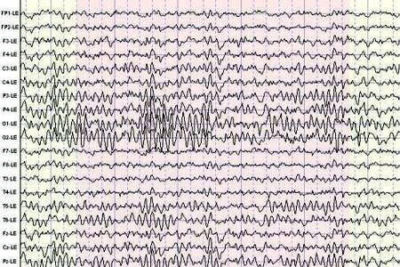
Depending on both its severity and location it can cause a variety of post-TBI cognitive, sensory and tactile, and motor impairments. Other challenges faced include identifying malingerers from genuine individuals with post-TBI morbidity, defining the severity of previous TBI in the field or previous injuries when reports are lost. Anticipating and preventing secondary injury and seizures post-trauma, defining severity of TBI, predicting TBI outcomes and arousal from coma or declaration of vegetative state or brain death form pivotal checkpoints in TBI management. It is a major health issue, very often fatal and causing high morbidity, changing the lives of both the person injured and the families involved. The results are reported on the same day, and sent to both your referring doctor and Dr Granot.Ī diagram of the EEG recorded from the electrodes on the patient’s scalp.Traumatic brain injury (TBI) can be caused by accidents like road traffic accidents (RTA), sports injuries, and injuries at home. The brain waves themselves may show asymmetries, suggesting there may be an underlying structural problem in the brain, as well as changes that show medication side effects and occasionally suggest dementia or brain dysfunction, such as delirium. Different types of spikes seen on the EEG Temporal lobe and other types of epilepsy will be diagnosed, together with the clinical symptoms, with changes such as spikes and spike-wave complexes. The EEG shows a number of different abnormalities that help with diagnosing different problems. What does the recording show? When will I know the results? The sleep deprived EEG lasts an hour (as the recording is longer, to give you time to fall asleep).Īfterwards, patients often go to wash their hair, due to some paste being left over. The routine EEG lasts around 40 minutes, including the time to put and take off the electrodes. As such, it is advised that you do not drive yourself to the EEG recording. This procedure will bring out epilepsy more readily. That means going to bed and then waking up very early, say 2AM, and staying awake for the rest of the night (without coffee or other stimulants), so that you come in to have the EEG (lying down this time) and ideally fall asleep (for at least a part of the recording).
These are important procedures to do during the EEG, as they can bring out different types of epilepsy and therefore help diagnose your problem better, so they are useful to undertake as best you can.Ī photo of EEG electrodes applied on the patient’s scalp.Īt times, to get more information, you will be asked to have an EEG done after sleep deprivation. During the EEG, you will be asked to do a few things, including opening and closing your eyes, breathing more rapidly (hyper-ventilating) as well as closing your eyes whilst bright light flashes. We will then record your brain waves and later analyse them. For a sleep deprived EEG, read on below.Ī total of 23 electrodes (gold plated small discs) will be applied to your scalp with sticky conductive paste. To prepare, please come in with clean, dry hair. It can also be used to help with looking after patients with dementia, head injury among others. This is the most common reason to be sent for an EEG, to help decide if episodes of collapse, fainting, blank staring or other sensations (abrupt fear, deja vu) may be related to epilepsy. It is used mainly to help diagnose epilepsy. The EEG (or electroencephalogram) is a test recording your brainwaves. On this page, I will discuss what an EEG (electroencephalogram) is used for, what you will feel during the test and a little bit about what it actually records.
